NIH Award Funds Data Coordinating Center for Down Syndrome Research
November 9th, 2020 by Global Down Syndrome Foundation
The new initiative will fuel collaboration and discovery about the biology of Down syndrome and its co-occurring medical conditions
Press Contacts:
Amanda Hilll Linda Crnic Institute for Down Syndrome | amanda.a.hill@cuanschutz.edu | C: 303.724.9907
Bobby Moulder Center for Data Driven Discovery in Biomedicine | moulderr@email.chop.edu | C: 484.258.8539
Hsiao-Ching Chou Sage Bionetworks | chou@sagebionetworks.org | C: 206.696.3663
DENVER, CO November 5, 2020 Scientists and data experts are joining forces to create the world’s first centralized platform for Down syndrome researchers to share, access, and analyze data. The goal of the new initiative, called the “Data Management and Portal for INCLUDE (DAPI) Project,” is to accelerate discoveries and advance medical care for individuals with Down syndrome. The National Institutes of Health (NIH) recently awarded a grant totaling $19.5M over five years to develop the center as part of the INCLUDE Project (INvestigation of Co-occurring conditions across the Lifespan to Understand Down syndromE).
The DAPI Project is co-led by Dr. Adam Resnick, Director of the Center for Data Driven Discovery for Biomedicine (D3b) at Children’s Hospital of Philadelphia, Dr. Joaquin Espinosa, Executive Director of the Linda Crnic Institute for Down Syndrome at the University of Colorado Anschutz Medical Campus, and Dr. Justin Guinney, Vice President of Computational Oncology at Sage Bionetworks. DAPI Project leaders will work closely with NIH INCLUDE Project staff to develop the center. This collaboration brings together strong expertise in Down syndrome research and open, data-driven science.
“We expect this new data center will be an impactful resource for the INCLUDE Project and the larger Down syndrome research community,” said Dr. Charlene Schramm, NIH Program Officer for the award. “The goal is to create a world-class portal for data sharing and analysis that will encourage innovative investigations into Down syndrome comorbidities across the lifespan.”
Dr. Melissa Parisi, one of the leaders of the NIH INCLUDE Project, added “The DAPI Project will combine data from existing research cohorts of individuals with Down syndrome with new cohorts. By building common data and shared analytic platforms, this project hopes to create a rich resource to help advance our understanding of these co-occurring conditions and support future therapeutic development.”
The INCLUDE Project is a trans-NIH initiative launched in 2018 to support research into conditions that affect individuals with Down syndrome and the general population. More than six million individuals living with Down syndrome have an increased risk of developing a wide range of medical conditions, such as certain autoimmune disorders and Alzheimer’s disease. At the same time, they are protected from some of the largest killers of the general population, including solid cancers and certain heart disease. Therefore, a key goal of the INCLUDE Project is to decode the underlying biology that alters these and many other co-occurring medical conditions in individuals with Down syndrome.
“Coordinated discovery efforts in this population not only have the potential to directly improve the lives of individuals with Down syndrome, but also to impact millions of other people affected by numerous related and co-occurring conditions,” said Dr. Espinosa of the Crnic Institute.
To enable these investigations, the mission of the DAPI Project is to create a world class platform for data sharing, data access, and integrative analysis in Down syndrome. The platform will empower scientists, physicians, and the community with tools to elicit evidence-based action in the laboratory, clinic, classroom, government, and society at-large.
“More and more, the scientific community is demonstrating the power of platforms to connect different communities with diverse areas of expertise and datasets to drive surprising discoveries and accelerated impact across a broad number of conditions in both children and adults,” said Dr. Resnick of D3b. “The DAPI Project will build on these efforts through the implementation of new technologies and platforms that will empower large-scale, diverse INCLUDE datasets on behalf of individuals with Down syndrome and other associated medical conditions and diseases.”
The DAPI Project is organized into three cores, roughly centered at each of the three partner organizations:
- Data Portal Core.Led by Dr. Resnick at D3b, the Data Portal Core oversees the development of the web-based data portal, which will be the public-facing centralized platform for data sharing and analysis. Dr. Resnick and the team at D3b are recognized leaders in collaborative, data-driven science, with expertise in pediatric cancers and diseases and large-scale data visualization and analysis.
- Data Management Core. Led by Dr. Guinney at Sage Bionetworks, the Data Management Core directs the overall data management practices for the DAPI Project, including protocols for data collection, governance, harmonization, processing, and sharing. Sage Bionetworks is a non-profit biomedical research organization devoted to responsible, open data-sharing practices, with broad expertise in computational and systems biology, as well as neurodegenerative diseases.
- Administrative and Outreach Core.Led by Dr. Espinosa at the Crnic Institute, the Administrative and Outreach Core leads outreach, education, and stakeholder engagement efforts for the scientific and Down syndrome communities, as well as overall project management. Dr. Espinosa and the Crnic Institute team are leading Down syndrome researchers who also administer a large Down syndrome research program at the University of Colorado.
Additional experts from Centre Hospitalier Universitaire Sainte-Justine, Oregon Health and Science University, Oregon State University, Seven Bridges Genomics, and Vanderbilt University Medical Center will also collaborate with the DAPI Project team.
“We have created a truly exceptional team with diverse expertise to accomplish the mission of the DAPI Project,” said Dr. Guinney of Sage Bionetworks. “We are all excited and honored to work with the NIH, the Down syndrome research community, and each other on this new endeavor.”
DAPI Project operations began in early October, including efforts to identify existing Down syndrome cohorts and data already established by researchers, to engage in ‘listening tours’ to understand the needs of the researcher and Down syndrome communities, and to develop frameworks for data governance, standardization, and management. The DAPI Project team aims to release the first version of the public data portal in 2022, while continuing to refine and expand the platform thereafter.
About the Center for Data Driven Discovery in Biomedicine (D3b)
The Center for Data Driven Discovery in Biomedicine (D3b) is a translational biomedical research Center of Emphasis at the Children’s Hospital of Philadelphia Research Institute. D3b’s multi-disciplinary expertise is accelerating bench-to-bedside research on behalf of children diagnosed with cancer and other rare conditions. D3b’s seven collaborative units bring together experts in oncology and basic research, genomics, data science, bioinformatics, neurosurgery, and other research-related disciplines to discover breakthroughs for every child, every time, everywhere. To learn more about the D3b Center, visit https://d3b.center/.
About the Linda Crnic Institute for Down Syndrome
The Linda Crnic Institute for Down Syndrome is the first academic research center fully devoted to improving the lives of people with Down syndrome through advanced biomedical research, spanning from basic science to translational and clinical investigations. Founded through the generous support and partnership of the Global Down Syndrome Foundation, the Anna and John J. Sie Foundation, and the University of Colorado, the Crnic Institute administers a thriving Down syndrome research program involving over 50 research teams across four campuses on the Colorado Front Range. To learn more, visit www.crnicinstitute.org or follow us on Facebook and Twitter @CrnicInstitute.
About Sage Bionetworks
Sage Bionetworks is a nonprofit biomedical research and technology development organization that was founded in Seattle in 2009. Our focus is to develop and apply open practices to data-driven research for the advancement of human health. Our interdisciplinary team of scientists and engineers work together to provide
researchers access to technology tools and scientific approaches to share data, benchmark methods, and explore collective insights, all backed by Sage’s gold-standard governance protocols and commitment to user- centered design. Sage is a 501c3 and is supported through a portfolio of competitive research grants, commercial partnerships, and philanthropic contributions. To learn more, visit https://sagebionetworks.org.
About Global Down Syndrome Foundation
The Global Down Syndrome Foundation (GLOBAL) is the largest non-profit in the U.S. working to save lives and dramatically improve health outcomes for people with Down syndrome. GLOBAL has donated more than $32 million to establish the first Down syndrome research institute supporting over 400 scientists and over 2,000 patients with Down syndrome from 28 states and 10 countries. Working closely with Congress and the National Institutes of Health, GLOBAL is the lead advocacy organization in the U.S. for Down syndrome research and care. GLOBAL has a membership of over 100 Down syndrome organizations worldwide, and is part of a network of Affiliates – the Crnic Institute for Down Syndrome, the Sie Center for Down Syndrome, and the University of Colorado Alzheimer’s and Cognition Center – all on the Anschutz Medical Campus.
GLOBAL’s widely-circulated medical publications include GLOBAL Medical Care Guidelines for Adults with Down Syndrome, Prenatal Testing and Information about Down Syndrome, and the award-winning magazine Down Syndrome WorldTM. GLOBAL also organizes the Be Beautiful Be Yourself Fashion Show, the largest Down syndrome fundraiser in the world. Visit globaldownsyndrome.org and follow us on social media (facebook & twitter:@GDSFoundation)(instagram:@globaldownsyndrome).
ON THE SCIENCE FRONTLINES: DOWN SYNDROME RESEARCH AT THE CRNIC INSTITUTE IS HELPING FIGHT AGAINST COVID-19
October 22nd, 2020 by Global Down Syndrome Foundation
From Down Syndrome WorldTM 2020 Issue 2 of 4
AMID A WORLD-WIDE PANDEMIC, THESE SCIENTISTS HAVE FOUND THEMSELVES IN A UNIQUE POSITION TO HELP, THANKS TO YEARS OF STUDYING THE EXCEPTIONAL BIOLOGY OF PEOPLE WITH DOWN SYNDROME.

This article was published in the award-winning Down Syndrome World™ magazine. Become a member to read all the articles and get future issues delivered to your door!
CONTRIBUTING IN A MEANINGFUL WAY to the body of science and medical practice surrounding an unprecedented world-wide pandemic is not something most people ever get the opportunity to do. It certainly was not what Executive Director of the Linda Crnic Institute for Down Syndrome, Dr. Joaquín Espinosa, and his team of scientists were thinking about in early March 2020.
During this time, the University of Colorado Anschutz Medical Campus (CU) shut down all research operations, locking scientists out of their buildings and laboratories in response to and to prevent the spread of the novel coronavirus (COVID-19) pandemic. Thankfully, Dr. Espinosa and the Crnic Institute team had their valuable experiments and supplies already gathered and stored away safely. With numerous grants from the National Institutes of Health (NIH), the National Science Foundation, and others, the team had plenty of work that could be performed remotely – analyzing data, writing up results for scientific journals, and preparing new proposals for funding.
Their biggest worry was something they could not work on remotely – the delay of their NIH clinical trial grant to treat autoimmune diseases in people with Down syndrome. In 2016, shortly after launching the Crnic Institute Human Trisome ProjectTM (HTP), the Crnic Institute made one of the most important scientific discoveries – Down syndrome can and should be characterized as an immune system disorder.
In particular, they discovered that an immune system pathway called the “interferon pathway” was “lit up” in people with Down syndrome pretty much 24/7, versus in typical people where it is only turned on when they are fighting a virus or infection and then it turns off.
The constant taxation of the immune system in people with Down syndrome creates low intensity inflammation that over time probably contributes to the co-occurrence of various diseases, including dementia. The Crnic Institute discovery was even more consequential because there are FDA-approved drugs that turn down the interferon pathway in typical people. Crnic Institute scientists were about use one of these FDA-approved drugs, a JAK inhibitor called tofacitinib, in an unprecedented clinical trial for adults with Down syndrome when the pandemic forced lab closures around the world.
AN “AH HA” MOMENT
As serendipity would have it, two days into quarantine, the Crnic team was doing a quick review of the research literature on COVID-19. Their findings revealed something that was both shocking and yet made perfect sense – it appeared that hospitalized COVID-19 patients were displaying many of the same patterns of immune system dysregulation that the Crnic Institute team had spent years studying, analyzing, and annotating in people with Down syndrome.
In COVID-19, the body’s antiviral defense system, which utilizes the interferon pathway, is sent into overdrive, causing the release of high levels of inflammatory signaling molecules known as cytokines. In COVID-19 and other viral infections, this “cytokine storm” is associated with respiratory distress, heart damage, and higher mortality rates. Similarly, people with Down syndrome have higher-than-normal levels of interferon signaling and often display more of a mini cytokine storm, even without a viral infection. Crnic Institute scientists believe this could contribute to many of the hallmarks of and co-occurring medical conditions associated with Down syndrome and are working to understand those connections.
Within a week, Dr. Espinosa and the Crnic Institute were one of a handful of research teams allowed back, with COVID-19 safety measures, into their labs to work on COVID-19 treatments for the general populations and to understand the connection and possible affects and treatments on people with Down syndrome.
Today, Dr. Espinosa is the leader of an international consortium looking at JAK inhibitors to treat COVID-19. The treatment is one of several clinical trials that Dr. Anthony Fauci, Director of the National Institute of Allergy and Infectious Disease at the NIH, has been supporting in the United States. The international consortium includes labs from the United States, China, Italy, France, Spain, Argentina, Mexico, Canada, Germany, and Denmark.
COVID-19 COULD BE MORE SEVERE FOR PEOPLE WITH DOWN SYNDROME
In reviewing the COVID-19 literature, Crnic Institute scientists also realized that people with Down syndrome should probably be considered a “high-risk” group for COVID-19. “High risk” means a person who gets COVID-19 has a higher probability of experiencing more severe illness than a member of the general population without other risk factors. This idea rests on the basis that the strength of the cytokine storm in COVID-19 correlates with disease severity and outcomes, and that people with Down syndrome will be more likely to develop a stronger, more prolonged cytokine storm due to higher levels of baseline interferon signaling. Although the direct studies of COVID-19 in Down syndrome needed to prove or disprove this idea have not yet been performed, ample supporting evidence already exists in the context of other viruses and in our basic understanding of immunology in Down syndrome.
It is also important to consider that people with Down syndrome have increased susceptibility to bacterial pneumonia. Although seemingly unrelated, it has been well documented that pandemics of respiratory viral infections are followed by a surge in cases of bacterial pneumonia, and that a large portion of deaths are actually attributed to secondary bacterial infections. Children with Down syndrome have much higher rates of viral pneumonia and bacterial pneumonia, with the latter being a leading cause of mortality in adults. Taken together, these known phenomena suggest that a person with Down syndrome who contracts COVID-19 would have an increased risk of also acquiring bacterial pneumonia.

PUTTING TOGETHER ALL THE EVIDENCE:
#1 – People with Down syndrome have higher levels of interferon signaling.
#2 – Once infected, people with Down syndrome have an increased risk of experiencing a stronger cytokine storm and thus a more severe case of COVID-19.
#3 – Both during and after infection with SARS-CoV-2, people with Down syndrome will be more likely to also contract bacterial pneumonia.
It is important to note that these are hypotheses and predictions based on existing evidence outside of COVID-19 and should be taken into consideration with caution. The studies needed to fully understand COVID-19 in people with Down syndrome are still just starting to get underway. The good news is, there are people with Down syndrome, with and without underlying conditions, who are surviving COVID-19. We simply need more data and to better understand this virus before we can definitively come to conclusion.
HOW DOWN SYNDROME RESEARCH FROM THE CRNIC INSTITUTE IS BEING UTILIZED TO STUDY AND TREAT COVID-19
Since March, every member of Dr. Espinosa’s team, from the basic scientists to the clinical researchers, and even the administrators, have been utilizing their unique skills and knowledge gained while working in Down syndrome to rapidly advance COVID-19 research at CU.
For example, Crnic Institute scientists immediately started testing potential therapeutics for the COVID-19 cytokine storm in their mouse model of Down syndrome, nicknamed Dp16. They weren’t actually exposing the Dp16 mice to SARS-CoV-2; they didn’t need to. Instead, the scientists could activate the immune system and stimulate a cytokine storm much like what is seen in COVID-19, simply by using a molecule that tricks the immune system into sensing a virus when there isn’t one. Crnic scientists then treat the mice with JAK inhibitors targeting the interferon signaling pathway that is chronically activated in people with Down syndrome and that drives the cytokine storm in COVID-19. The data resulting from these experiments will be extremely valuable because it can be interpreted and utilized in two contexts: COVID-19 and Down syndrome.
FIGHTING COVID-19 TOGETHER
Who would have ever guessed that Down syndrome research and the discovery that interferon signaling is chronically activated in people with Down syndrome would one day so greatly impact the science and research behind a historic, global pandemic? This meaningful contribution to the body of science and medical practice surrounding COVID-19 is something the Down syndrome community should be proud to be part of. Together, this community of researchers, self-advocates, families, and supporters can clearly make positive scientific impacts not only for people with Down syndrome, but also for the entire world.
THE CRNIC INSTITUTE HUMAN TRISOME PROJECTTM IN ACTION AGAINST COVID-19
At the beginning of the quarantine, CU assembled a centralized team tasked with rapidly creating a biobank to collect blood and other biological samples from COVID-19 patients. These samples would then be administered to researchers with approved projects. This model essentially replicates one of the Crnic Institute’s flagship research initiatives, the Crnic Institute Human Trisome ProjectTM (HTP). The HTP is generating multiple layers of “omics” data (think big data from sequencing all of someone’s DNA and RNA and measuring all their proteins, metabolites, immune cells, and much more) on hundreds of people with and without Down syndrome in order to understand the hallmarks of and co-occurring medical conditions associated with Down syndrome. Having heard about the Crnic Institute’s HTP and Biobank, the CU COVID-19 team reached out to Crnic scientists to tap into their expertise. The Crnic team shared detailed protocols and helped advise the CU team during the development of the CU COVID-19 Biobank.
As part of a synergized endeavor with the COVID-19 Biobank, leading researchers at CU also partnered with Dr. Espinosa and the Crnic team to replicate the experimental platform from HTP and apply it to COVID-19. The parallel effort by CU to apply the HTP platform to COVID-19 has been aptly dubbed “The COVIDome Project,” and Crnic scientists are leading the ongoing data generation to advance COVID-19 research for better diagnostics and therapeutics.
The Crnic team is also partnering with a national COVID-19 collaborative group to specifically study COVID-19 in people with Down syndrome. As explained earlier in this article, so much is yet unknown about COVID-19 in Down syndrome and numerous studies are needed to understand its impacts. The team is working with top data scientists at CU to identify differences in risk factors, symptoms, clinical course, immunological parameters, response to various treatments, and outcomes and long-term effects of COVID-19 in people with Down syndrome. Alongside these efforts, the Crnic team is also studying individuals with Down syndrome who have recovered from a SARS-CoV-2 infection as part of the HTP, in order to assess changes induced by COVID-19 across all the layers of omics data. Together, Crnic scientists hope these efforts will advance our understanding of interferon signaling and the cytokine storm in COVID-19 and Down syndrome and
inform the development of customized preventative and therapeutic solutions.

Like this article? Join Global Down Syndrome Foundation’s Membership program today to receive 4 issues of the quarterly award-winning publication, plus access to 4 seasonal educational Webinar Series, and eligibility to apply for Global’s Employment and Educational Grants.
Register today at downsyndromeworld.org!
Global Down Syndrome Foundation Announces The 1st Evidence-Based Medical Care Guidelines For Adults With Down Syndrome
October 20th, 2020 by Global Down Syndrome Foundation
The Global Guideline is Published in the Print & Online Versions of JAMA,
Ensuring Clinicians Across the U.S. Have Access
Press Contacts:
Anca Call | acall@globaldownsyndrome.org | C: (720) 320-3832
Rejena Carmichael | rcarmichael@globaldownsyndrome.org | C: (240) 603-5494
October 20, 2020 Denver, CO – After four years of coordination, compilation, and rigorous assessment and writing, the Global Down Syndrome Foundation Medical Care Guidelines for Adults with Down Syndrome© (Global Guideline) is complete and available at no cost.
The authors include the clinical directors of eight of the largest adult Down syndrome medical centers in the country – Advocate Health Care in Chicago, University of Pittsburgh Medical Center, Kennedy Krieger Institute at Johns Hopkins School of Medicine, University of Kansas Medical Center, University of Arkansas for Medical Sciences, and Denver Health in conjunction with the Anschutz Medical Campus School of Medicine at University of Colorado.
The first-in-kind Global Guideline was peer reviewed, edited, and published in the Special Communication section of the print and online October 2020 issue of JAMA, the Journal of the American Medical Association.
“We are so pleased that the quality of our guideline rose to the occasion of being published in JAMA, and we are deeply grateful to our families and self-advocates for pushing us to work on this difficult project,” says Michelle Sie Whitten, President & CEO of the Global Down Syndrome Foundation (GLOBAL). “Now we can focus on collaborating with other Down syndrome and disability organizations as well as medical institutions to ensure clinicians are following our Global Guideline and measuring outcomes.”
The Global Guideline is for clinicians and addresses nine medical areas: Behavioral Health, Dementia, Diabetes, Cardiovascular Disease, Obesity, Atlantoaxial Instability, Osteoporosis, Thyroid, and Celiac Disease.
It is made up of 14 recommendations and 4 statements of good practice. Some of the recommendations align with existing guidelines for individuals without Down syndrome, and two are markedly different. There were several questions associated with the recommendations that had no published research evidence, and therefore were answered based on the clinical expertise of the authors.
“It’s clear that the lack of Down syndrome research funding over the last 20 years has prevented us from easily or quickly creating these guidelines,” says Bryn Gelaro, LSW, Director of Adult Initiatives & Special Projects at GLOBAL. “We were fortunate to have expert authors and volunteers who helped identify important research needs that will bolster and better define our future Global Guideline recommendations.”
Author Amy Tsou, MD, from ECRI, an independent nonprofit and Evidence-based Practice Center, with support from Gelaro, helped spearhead the research methodology, which included PICO (Population/Intervention Comparison/Outcome) questions, the GRADE (Grading of Recommendations, Assessment, Development, and Evaluation) methodology, and focus groups from various stakeholders informed the final draft.
“I participated in the task force of over 40 self-advocates and family members that provided GLOBAL with the directive they needed to focus on adult care guidelines – even if it would be difficult and take a lot of time,” says Karen Gaffney, a nationally renowned athlete, GLOBAL Q-Awardee and spokesperson. “It was great to be able to participate in the week-long focus group of self-advocates and family members and see it all come together.”
“From the beginning, GLOBAL has been leading the way, empowering people with Down syndrome with improved care and health outcomes,” says mom Darlene Beals. “The Global Guideline is an important new resource for my 24-year-old son Alan, and I believe if anyone can get to the bottom of health disparities for African Americans with Down syndrome, it’s GLOBAL.”
Alan echoes his mom’s sentiments, “[I want to know] when to take thyroid medicine, once a day? How to live a healthy life in my own apartment and keep the apartment clean?” Alan is also concerned about doctors knowing how to pay Medicaid insurance.
While the Global Guideline is free of charge to any stakeholder, the copyright of the JAMA publication and of GLOBAL’s long-form publication prohibits the reproduction of the Global Guideline on any website or digital platform. However, printing and downloading for personal and clinical use is highly encouraged.
GLOBAL has support from over 50 local, national, and international Down syndrome organizations and several generous sponsors. By the end of 2021, GLOBAL plans to translate and distribute this transformative new resource into several languages, and to update and expand the Global Guideline every 6 years.
A webinar and Q&A with the renowned and expert authors will be held on Wednesday, October 21, 2020. To learn more or sign up, please click here.
The Global Down Syndrome Foundation Medical Care Guidelines for Adults with Down Syndrome Workgroup includes (in alphabetical order of lead and supporting authors):
- Peter Bulova, MD: Associate Professor of Medicine, University of Pittsburgh Medical Center, Pittsburgh, Pennsylvania
- George Capone, MD: Director, Down Syndrome Clinic & Research Center, Kennedy Krieger Institute, Associate Professor of Pediatrics, Johns Hopkins School of Medicine, Baltimore, Maryland
- Brian Chicoine, MD: Medical Director, Advocate Medical Group Adult Down Syndrome Center, Park Ridge, Illinois
- Terry Odell Harville, MD, PhD, D(ABMLI) D(ABHI): Professor of Pathology and Laboratory Services, and Internal Medicine, Department of Pathology and Laboratory Services, and Department of Internal Medicine, Division of Hematology, University of Arkansas for Medical Sciences, Little Rock, Arkansas
- Barry A Martin, MD: Associate Professor of Clinical Practice, Division of General Internal Medicine, University of Colorado School of Medicine, Anschutz Medical Center, Aurora, Colorado
- Dennis McGuire, LCSW, PhD: Private Practice, Evanston, Illinois
- Kent D. McKelvey, MD: Associate Professor, Rockefeller Chair in Clinical Genetics, University of Arkansas for Medical Sciences, Little Rock, Arkansas
- Moya Peterson, PhD, APRN, FNP-BC: Clinical Professor, University of Kansas Medical Center, Schools of Nursing and Medicine, Kansas City, Kansas
- Amy Y Tsou, MD, MSc: Evidence-based Practice Center, ECRI Center for Clinical Excellence and Guidelines, Plymouth Meeting, Pennsylvania; Staff Neurologist, Division of Neurology, Michael J Crescenz Veterans Affairs Medical Center, Philadelphia, Pennsylvania
- Carl Tyler, MD, MSc: Director of Developmental Disabilities – Practice-Based Research Network, and Professor, Family Medicine and Community Health, Cleveland Clinic Lerner College of Medicine, Case Western Reserve University School of Medicine, Cleveland, Ohio
- Michelle Sie Whitten, MA: President & CEO, Global Down Syndrome Foundation, Denver, Colorado
- Bryn Gelaro, MA, LSW: Director of Adult Initiatives, Global Down Syndrome Foundation, Denver, Colorado
- Michael Wells, BS: Formerly Research Coordinator, Developmental Disabilities – Practice-Based Research Network, Cleveland, Ohio
About the Global Down Syndrome Foundation
The Global Down Syndrome Foundation (GLOBAL) is the largest non-profit in the U.S. working to save lives and dramatically improve health outcomes for people with Down syndrome. GLOBAL has donated more than $32 million to establish the first Down syndrome research institute supporting over 400 scientists and over 2,000 patients with Down syndrome from 28 states and 10 countries. Working closely with Congress and the National Institutes of Health, GLOBAL is the lead advocacy organization in the U.S. for Down syndrome research and care. GLOBAL has a membership of over 150 Down syndrome organizations worldwide, and is part of a network of Affiliates – the Crnic Institute for Down Syndrome, the Sie Center for Down Syndrome, and the University of Colorado Alzheimer’s and Cognition Center – all on the Anschutz Medical Campus.
GLOBAL’s widely-circulated medical publications include GLOBAL Medical Care Guidelines for Adults with Down Syndrome, Prenatal Testing and Information about Down Syndrome, and the award-winning magazine Down Syndrome WorldTM. GLOBAL organizes the Be Beautiful Be Yourself Fashion Show, the largest Down syndrome fundraiser in the world. Visit globaldownsyndrome.org and follow us on social media (Facebook, Twitter @GDSFoundation, Instagram @globaldownsyndrome).
Pioneering Care for People with Down Syndrome
November 8th, 2018 by Global Down Syndrome Foundation

From Down Syndrome World Issue 3 2018
As one of the lead authors of the Medical Care Guidelines for Adults with Down Syndrome, George T. Capone, M.D., is continuing his life’s work of improving evidence-based medical care for people with Down syndrome.
 FOR THE PAST 30 YEARS, George T. Capone, M.D., has specialized in providing quality care for patients with Down syndrome, always pushing for better evidence-based treatment and interventions. As a research scientist, Director of the Kennedy Krieger Institute’s Down Syndrome Clinic and Research Center (DSCRC), and Associate Professor of Pediatrics at the Johns Hopkins University School of Medicine, he has seen more than 2,500 patients, ranging in age from infants to seniors. Dr. Capone has contributed to improved care since the 1980s, and he continues to be concerned about health care for adults with Down syndrome.
FOR THE PAST 30 YEARS, George T. Capone, M.D., has specialized in providing quality care for patients with Down syndrome, always pushing for better evidence-based treatment and interventions. As a research scientist, Director of the Kennedy Krieger Institute’s Down Syndrome Clinic and Research Center (DSCRC), and Associate Professor of Pediatrics at the Johns Hopkins University School of Medicine, he has seen more than 2,500 patients, ranging in age from infants to seniors. Dr. Capone has contributed to improved care since the 1980s, and he continues to be concerned about health care for adults with Down syndrome.
Dr. Capone’s extensive knowledge, experience, and passion to improve care are the primary reasons he was tapped to join a team of physicians and researchers updating the Medical Care Guidelines for Adults with Down Syndrome, a project funded by the Global Down Syndrome Foundation.
AN EARLY SUPPORTER OF TRANSLATIONAL RESEARCH
Dr. Capone’s career treating people with Down syndrome took root in 1988, when he began a neurobiology fellowship at Johns Hopkins University School of Medicine. At the time, researchers at Johns Hopkins, including his mentor Joseph T. Coyle, M.D., were conducting groundbreaking genetic research on the link between Down syndrome and Alzheimer’s disease. Among the many projects he saw occurring in Dr. Coyle’s lab was research that used TS16 mouse models to investigate the impact that three copies of chromosome 21 — the defining characteristic of Down syndrome — has on early-onset Alzheimer’s disease. It was some of the earliest research on the subject.
 This article was published in the award-winning Down Syndrome World™ magazine. Become a member to read all the articles and get future issues delivered to your door!
This article was published in the award-winning Down Syndrome World™ magazine. Become a member to read all the articles and get future issues delivered to your door!The time spent in Dr. Coyle’s lab helped lay the foundation for Dr. Capone’s interest in how that research could be directly applied to the health and well-being of patients. In the early 1990s, Dr. Capone joined the Kennedy Krieger Institute. There, he recognized that the DSCRC provided ample opportunity to develop hypotheses and research questions on the neurobiological and neurobehavioral basis of cognitive impairment associated with Down syndrome. The clinic’s diverse patient population allowed for “person-centered clinical research focusing on the medical and mental health conditions we see on a daily basis.” Such research, he knew, would benefit not only people with Down syndrome but also patients with its co-occurring conditions, such as Alzheimer’s disease, sleep apnea, and heart conditions.
Under Dr. Capone’s leadership, the DSCRC has conducted studies on a range of conditions, including autism-spectrum disorders and attention-deficit/hyperactivity disorder. His research has led to the characterization of autism in children with Down syndrome, uncommon neurobehavioral and developmental profiles of children and teenagers with Down syndrome, and developmental regression in people of all ages with the condition.
He has also designed and conducted several clinical pharmacology trials for drugs intended to improve memory and cognition in both children and adults, including risperidone, guanfacine, and rivastigmine.
“The science is fascinating, and the associated medical conditions are complex and perplexing,” Dr. Capone said. “The families I work with are the best, and the children and adults I interact with always amaze me.”
FORGING NEW PATHS FOR ADULT MEDICAL CARE
Dr. Capone agrees that the increased knowledge and advocacy among parents and healthcare professionals, the establishment of specialized clinics such as the DSCRC, and advancements in medical-surgical care for children have all progressed health for people with Down syndrome. Yet, despite contributions to the field of care for people with Down syndrome, more research is necessary to improve lives.
“We need to better understand the etiology-pathogenesis and risk factors associated with certain medical conditions, as well as what treatment approaches and prevention strategies are most beneficial to our patients,” Dr. Capone explained. “We also need a more organized approach to managing data sets to improve clinical decision-making, patient and caretaker outcomes, and quality of life.”
The Medical Care Guidelines for Adults with Down Syndrome will go a long way toward improving clinical decision-making and health outcomes. The current guidelines available for adults with Down syndrome were last updated in 2001 and do not adequately reflect the more than doubling of life span for people with Down syndrome since the 1980s. As adults with Down syndrome are living longer, they require care specific to their unique aging experience and risk factors.
“Many physicians in adult medicine do not have adequate training to care for people with genetic and neurodevelopmental conditions,” Dr. Capone said. “The medical conditions experienced by adults with Down syndrome can appear overwhelming and beyond the reach of many physicians, but with sufficient resources and training, we can teach primary care and other adult healthcare providers how to provide this care with confidence.
“Coming up with medical care guidelines will expose how little we really know about ‘best practices’ when caring for aging adults with Down syndrome and chronic medical conditions,” he added. “I hope it will stimulate further interest and investigation into this often neglected aspect of clinical research.”
To learn more about the Medical Care Guidelines for Adults with Down Syndrome, please visit globaldownsyndrome.org/medical-care-guidelines.
ADVICE FOR FAMILIES AND SELF-ADVOCATES
George T. Capone, M.D., Director of the Down Syndrome Clinic and Research Center at Kennedy Krieger Institute and Associate Professor of Pediatrics at the Johns Hopkins University School of Medicine, has some advice, learned over a 30-year career, to pass along to people with Down syndrome and their families.
Don’t get caught up in comparisons.
“If your child seems different compared to other children you know with Down syndrome, don’t despair,” Dr. Capone said. “All our children are unique, and we should rejoice in these differences.”
Exercise body and mind.
“Stay physically and mentally active once you leave high school or post-secondary school,” he said. “Find your own means of self-expression through the performing arts, fitness, hobbies, and fun social activities.”
Connect.
“Stay informed and connected to the larger Down syndrome community of families and selfadvocates,” he advised.
Like this article? Join Global Down Syndrome Foundation’s Membership program today to receive 4 issues of the quarterly award-winning publication, plus access to 4 seasonal educational Webinar Series, and eligibility to apply for Global’s Employment and Educational Grants.
Register today at downsyndromeworld.org!
A Center For Life-Changing Care
October 12th, 2018 by Global Down Syndrome Foundation

From Down Syndrome World Winter 2017
Since its inception in 2010, The Anna and John J. Sie Center for Down Syndrome at Children’s Hospital Colorado has championed healthy starts and bright futures by caring for the unique medical needs of young people with down syndrome.
WHEN HER DAUGHTER, Sophia, was born with Down syndrome 13 years ago, Michelle Sie Whitten, President and CEO of the Global Down Syndrome Foundation, traveled more than 1,000 miles from her home in Denver to the Thomas Center for Down Syndrome Services at Cincinnati Children’s Hospital Medical Center to find the specialized medical care Sophia needed. After talking with other local families making the same trek, Whitten began exploring what it would take to bring a similar center to Colorado.
“The initial thinking was, ‘Why should we have to travel?’” Whitten said. “Why shouldn’t Colorado have a fabulous, world-class pediatric medical center for kids with Down syndrome?”
From Whitten’s due diligence and efforts, and funding from Sophia’s grandparents, Anna and John J. Sie, came the Sie Center, a medical center that opened in 2010 at Children’s Hospital Colorado as part of the Linda Crnic Institute for Down Syndrome.
PUTTING POTENTIAL WITHIN REACH
“There’s a lot of talk about people with Down syndrome reaching their full potential,” Whitten said. “At Global, we feel very strongly that without good health, you’ll never reach your full potential.”
Helping children and young adults up to age 21, the Sie Center’s team of medical professionals provides the expert care and resources needed to manage a wide range of physical and behavioral health issues associated with Down syndrome. These specialists work closely with primary care providers at Children’s Hospital Colorado to coordinate care and deliver services through seven clinics.
At the Medical Clinic, a developmental pediatrician, nurse, and physical therapist evaluate children’s medical issues and physical growth to develop a comprehensive care plan. During visits, kids may also see an occupational therapist as needed.
 This article was published in the award-winning Down Syndrome World™ magazine. Become a member to read all the articles and get future issues delivered to your door!
This article was published in the award-winning Down Syndrome World™ magazine. Become a member to read all the articles and get future issues delivered to your door!The Sie Center’s Feeding Clinic offers families an opportunity to visit with a feeding and swallowing specialist, developmental pediatrician or nurse practitioner, physical therapist, and social worker. These providers help parents address muscle weakness and other issues with eating and drinking that can interfere with a child’s ability to breast-feed, chew, and/or swallow and therefore raise his or her risk of silent aspiration.
The ENT Clinic helps manage diseases of the ear, nose, and throat, including chronic ear infections, airway obstructions, and hearing loss. Approximately 70 to 75 percent of kids with Down syndrome deal with hearing loss, according to the Eunice Kennedy Shriver National Institute of Child Health and Human Development.
The Sie Center is the first center of its kind to have a full-time School-Age Clinic. The clinic’s educational specialist and psychologist help families develop individualized education programs and identify medical problems that may contribute to difficulties with behavior and learning. For example, a child who is acting out in gym class may do so because his feet hurt — not because he doesn’t want to participate in the activity.
“These specialists are like medical detectives,” Whitten said. “They work very closely to understand what’s happening at school and what modifications, support, and resources may be helpful.”
Through the Infant Clinic, babies receive a complete evaluation of their physical health to identify medical needs at a very early age.
At the Sleep Clinic, physicians evaluate children for sleep disorders and help parents troubleshoot solutions for common challenges, such as using a continuous positive airway pressure machine.
Currently, the Telemedicine Clinic connects Sie Center specialists with providers in Durango, Colorado, who treat children with Down syndrome, but Whitten said the goal is to expand the service to benefit the maximum possible number of patients.
In addition to these clinics, the Sie Center recently instituted a mental wellness program. Often, young people experiencing regression or warning signs of depression and anxiety are told that these symptoms are complications related to Down syndrome. However, these issues may be treatable mental illnesses, just as they would be for typical young adults.
A GLOBAL IMPACT
The clinic’s specialists are actively involved in clinical research projects that will help doctors around the world improve care for children with Down syndrome.
Arwen Jackson, MA, CCC-SLP; Jennifer Maybee, OTR, MA, CCC-SLP; Maura K. Moran; Kristine Wolter-Warmerdam; and Francis Hickey, M.D., FAAP, all with the Sie Center or Children’s Hospital Colorado, published their latest study on aspir ation in the international journal Dysphagia.
“Doctors at Children’s Hospital Colorado are also joint appointees at the University of Colorado School of Medicine, so we’re able to get a lot of medical students who are required to do a fellowship or some kind of rotation,” Whitten said. “Working with the Sie Center gives them an in-depth look at the best way to provide medical care to patients with Down syndrome, and that carries over to the care they give in the future.
“The services the Sie Center provides are nothing short of life-changing, if not lifesaving,” Whitten added. “I’ve spoken with parents who’ve told me, ‘I was always afraid, but now that I’m at the Sie Center, I understand what’s going on. I know what I’m supposed to be doing for my child’s health.’”
CARE COUNTS
The Anna and John J. Sie Center for Down Syndrome at Children’s Hospital Colorado is one of the largest centers of its kind in the world. Here’s a snapshot of the clinic’s impact:
• More than 1,500 visits take place at the Sie Center each year.
• The Sie Center serves approximately 1,300 patients annually.
• The pediatricians, specialists, and therapists at the Sie Center have more than 80 years collective experience caring for children with Down syndrome.
• Families representing 26 states, seven countries, and Puerto Rico seek care at the Sie Center.
Global provides continued financial support for the Sie Center. Visit The Sie Center web page to learn how you can help efforts to provide medical care for children and young adults with Down syndrome.
Like this article? Join Global Down Syndrome Foundation’s Membership program today to receive 4 issues of the quarterly award-winning publication, plus access to 4 seasonal educational Webinar Series, and eligibility to apply for Global’s Employment and Educational Grants.
Register today at downsyndromeworld.org!
Two Global Down Syndrome Foundation Experts Receive Prestigious National Awards for Scientific Breakthrough and Contributions in the Medical Field
July 23rd, 2018 by Global Down Syndrome Foundation
Dallas, TX – Dr. Joaquín Espinosa, Ph.D., Executive Director of the Linda Crnic Institute for Down Syndrome on the Anschutz Medical Campus (Crnic Institute), was awarded the National Down Syndrome Congress 2018 Pueschel-Tjossem Award for his scientific breakthrough recasting Down syndrome as an immune system disorder. Dr. Dennis McGuire, LCSW, Ph.D., Senior Consultant for Adult Medical Initiatives at the Global Down Syndrome Foundation (Global), received the 2018 Down Syndrome Medical Interest Group William I. Cohen MD, Distinguished Service Award for his lifetime work in behavioral and mental health for adolescents and adults with Down syndrome. He received the award along with his esteemed and accomplished colleague, Dr. Brian Chicoine, M.D.. Both awards were presented at the National Down Syndrome Congress (NDSC) Annual Convention.
 Kishore Vellody, M.D., Frank Stephens, Joaquín Espinosa, Ph.D.,DeOndra Dixon, and David Tolleson
Kishore Vellody, M.D., Frank Stephens, Joaquín Espinosa, Ph.D.,DeOndra Dixon, and David Tolleson
Dr. Espinosa is a nationally and internationally renowned cancer scientist. As the Executive Director of the Crnic Institute, a Global Affiliate, he oversees the Crnic Institute Human Trisome Project™, studying how Down syndrome (trisomy 21) connects to cancer, Alzheimer’s, immune system disorders, and multiple other co-morbidities. He is also a Professor in the Department of Pharmacology and founding Director of the Functional Genomics Facility at the University of Colorado Anschutz Medical Campus School of Medicine, and co-Leader of the Molecular Oncology program at the University of Colorado Cancer Center. The NDSC Pueschel-Tjossem Award recognizes research that has contributed to greater knowledge and understanding of Down syndrome and has improved the lives of people with Down syndrome and their families.
 Dr. Dennis McGuire and Dr. Brian Chicoine
Dr. Dennis McGuire and Dr. Brian Chicoine
Dr. McGuire has more than 30 years of experience in the fields of mental health and developmental disabilities. He currently serves as Global’s Senior Consultant specializing in adult initiatives, including establishing a medical care center for adults with Down syndrome in Denver. Along with his colleague Dr. Chicoine, Dr. McGuire co-founded the Adult Down Syndrome Center of Lutheran General Hospital in Chicago, the largest, most prestigious clinic for adults with Down syndrome in the United States, where he served as Director of Psychological Services. Drs. McGuire and Chicoine co-authored two milestone books, Mental Wellness in Adults with Down Syndrome and The Guide to Good Health for Teens and Adults with Down Syndrome. Both doctors are serving as authors for Global’s Medical Care Guidelines for Adults with Down Syndrome – an important community service project.
The Down Syndrome Medical Interest Group-USA (DSMIG-USA) established the William I. Cohen, MD Distinguished Service Award in 2016 to honor a member for major contributions to DSMIG-USA’s mission of promoting the health and wellness of individuals with Down syndrome.
Colorado Public Radio interviews Global President & CEO on pivotal research that could improve lives
January 3rd, 2018 by Global Down Syndrome Foundation
Michelle Sie Whitten, who heads the Denver-based Global Down Syndrome Foundation, has big hopes for new research at the University of Colorado, where scientists say they have upended the conventional wisdom that Down syndrome is a brain disorder. Instead, they classify it as a malfunction of the immune system.
Improving Quality of Life for Adults with Down Syndrome
October 25th, 2017 by Global Down Syndrome Foundation
A Lifetime Of Good Health Begins With Evidence-Based Guidelines
In the U.S., the life expectancy of an individual with Down syndrome has more than doubled in the last three decades, from 25 years in 1983 to 60 years today.
The reason for this increased lifespan is two-fold. First, the inhumane institutions where the overwhelming majority of people with Down syndrome were forced to live were dismantled in the 1980s and 1990s. This dismantling was a product of the human and civil rights movements of the 1960s and 1970s, which resulted in children with Down syndrome being raised in their homes and receiving education and medical care — basic rights they were deprived of in institutions.
Second, in the 1980s, there were considerable advancements in pediatric heart surgeries, as well as a legal battle that rightly ended with doctors being required to perform lifesaving procedures, including open-heart surgery, for children with Down syndrome.
Although people with Down syndrome are enjoying a significantly increased lifespan, their longevity is revealing some challenging age-related medical diagnoses. For example, it is estimated that approximately 70 percent of people with Down syndrome will develop Alzheimer’s disease. As they age, they are also at increased risk of many immune system disorders and obesity. Conversely, they are highly protected from several diseases, including most solid tumor cancers, such as breast cancer, as well as certain types of heart attacks and strokes. It is clear that people with Down syndrome have a different disease spectrum than typical people.
The American Academy of Pediatrics does an excellent job of periodically updating guidelines pediatricians should follow for their patients with Down syndrome. However, the last medical care guidelines for adults with Down syndrome were published in 2001. They provide many excellent insights and recommendations, but are in need of updates based on the increased lifespan of people with Down syndrome and advances in medical science.
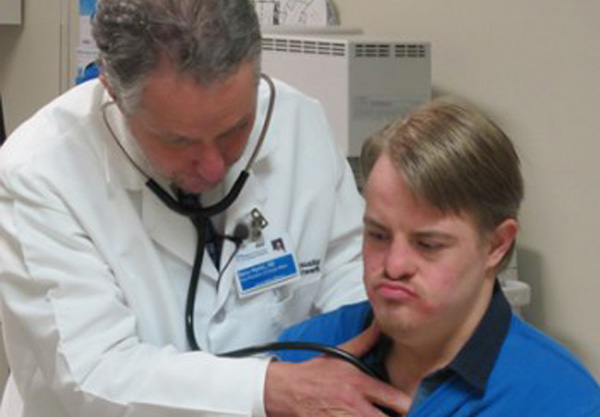
In 2015, the Global Down Syndrome Foundation’s Task Force for Adults with Down Syndrome, a team of more than 60 self-advocates, their family members, and medical professionals, unanimously voted for Global to make updating medical care guidelines for adults with Down syndrome a priority.
“The primary purpose is to improve the physical and behavioral health of, and medical care for, people with Down syndrome. That’s absolutely why we’re doing this,” said Dennis McGuire, Ph.D., LCSW,
Senior Consultant at Global. He helped create the first adult medical care guidelines and is tasked with helping galvanize some of the leading medical professionals in adult care to establish new, comprehensive guidelines. “When we’re talking about health care and behavioral health, we’re talking about improving people’s quality of life. That’s our goal.”
EMPOWERING DOCTORS TO PROVIDE BETTER CARE
The new Medical Care Guidelines for Adults with Down Syndrome will provide medical professionals with updated information about adults with Down syndrome and a checklist of recommended screenings and tests that cater to the unique medical profile of this special population.
 This article was published in the award-winning Down Syndrome World™ magazine. Become a member to read all the articles and get future issues delivered to your door!
This article was published in the award-winning Down Syndrome World™ magazine. Become a member to read all the articles and get future issues delivered to your door!Ideally, the guidelines will allow adults with Down syndrome to receive the best possible car e, regardless of where they live.
“There are only a few clinics in the entire country serving teens and adults with Down syndrome,” Dr. McGuire said. “So there are huge numbers of them without access to specialty care. They go to local doctors, who may see just a few people with Down syndrome over the course of a year. The guidelines can provide those physicians with a resource they can tr ust, which will help them deliver better care.”
ADDRESSING KEY AREAS OF MEDICINE
Initially, the new guidelines will cover medical car e across multiple disciplines, including cardiology, immunology, behavioral and mental health, and obesity/metabolism.
“We want to eventually cover many more areas,” said Michelle Sie Whitten, President and CEO of Global. “Unfortunately, Down syndrome is still one of the least-funded genetic conditions by our federal government. As a result, we won’t have enough evidence-based research to provide definitive guidelines in some areas but will rather be able to make recommendations. However, in identifying the research gaps, we can also prioritize such research so when we go back to update the guidelines in five years, we have targeted, more comprehensive research to rely on.”
“New health guidelines could prove beneficial for many reasons,” said Dr. McGuire, who worked for 25 years as a behavioral health expert at the Adult Down Syndrome Center at Advocate Lutheran General Hospital in Chicago. “For example, we’ve found that people with Down syndrome have a tendency toward depression. We also know there’s an overlap between physical and behavioral health. If people have thyroid problems, those can present as behavioral change. When people come in with changes in behavior, behavioral health professionals will recommend a thorough physical exam to make sure there are no physiological issues. If we’re treating depression without treating its physical causes, we’re not really helping [someone with Down syndrome].”
VETTING THE DATA
The first step in the creation of the new guidelines is a rigorous research process by the ECRI Institute, a nonprofit organization that conducts research to create evidence-based medical guidelines. ECRI works closely with the U.S. Department of Health and Human Services’ National Guideline Clearinghouse, which validates the guidelines.
“After that, we’ll gather information from the researchers and clinicians, put it into the form of actual guidelines, and make certain they are published in medical journals,” Dr. McGuire said. “ECRI’s role is to make sure that the quality of this process is extremely high.”
The project has attracted leading medical professionals from throughout the U.S. who provide clinical care to thousands of adult patients with Down syndrome every year. These clinicians will use the ECRI-vetted data as a basis to apply their vast knowledge in different areas and help craft guidelines and recommendations.
The entire process is expected to take two years, and the anticipated completion date is the end of 2018 with the guidelines being available for publication in early 2019.
A VALUABLE RESOURCE
The goal is to have the guidelines published in major medical journals to r each specialty fields and as many medical professionals as possible. The guidelines will be free to parents, caregivers, healthcare providers, and local Down syndrome organizations.
“Parents have always been, by far, the best advocates for people with Down syndrome,” Dr. McGuire said. “We’ve made certain to have a version available to families so they can use them to advocate for their sons and daughters .”
WORTH THE COST
The two-year-long process of creating the new Medical Care Guidelines for Adults with Down Syndrome is costly. Global Down Syndrome Foundation has committed to funding this important initiative, translating the guidelines into 10 languages, and updating them every five years. Global is reaching out to the Down syndrome community for donations, and so far, 28 Down syndrome organizations and multiple individuals have contributed. Their generosity will be recognized in the published guidelines.
“Research is expensive,” said Dennis McGuire, Ph.D., LCSW, Senior Consultant at Global. “Many groups have already stepped up to help fund the guidelines. They know how important this is and are very excited.”
Your ongoing support is crucial to ensuring the best-quality guidelines. To donate, visit
www.globaldownsyndrome.org/donate/
“Tens of thousands of people with Down syndrome reach adulthood each year, and this increases the importance of and need for evidence-based guidelines in this expanding group. Recommendations applied to a person with Down syndrome as a child may not be relevant in adulthood,” said Kent McKelvey, M.D., who leads the Adult Medical Genetics and Down Syndrome Clinic at the University of Arkansas for Medical Sciences. “The presence of three copies of chromosome 21 has implications for development and aging in every organ system. This seems logical and we have some understanding of the processes on a molecular level. We see patterns of disease predisposition with age but we have not translated this into a comprehensive medical management approach. A systematic process such as this is needed to find the gaps in the evidence and order the current evidence into usable guidelines for primary care doctors.”
Like this article? Join Global Down Syndrome Foundation’s Membership program today to receive 4 issues of the quarterly award-winning publication, plus access to 4 seasonal educational Webinar Series, and eligibility to apply for Global’s Employment and Educational Grants.
Register today at downsyndromeworld.org!
Global Down Syndrome Foundation Urges U.S. Senate To Maintain Important Patient Protections and Coverage As Part Of Health Reform Plan
June 26th, 2017 by Global Down Syndrome Foundation
Global Down Syndrome Foundation (Global) is a nonpartisan, leading research, medical care and advocacy organization for people with Down syndrome. Global believes strongly that all Americans, including members of our community, must have access to affordable, high-quality healthcare and health insurance coverage appropriate for their needs. Global urges Senators to keep key patient protections and health insurance coverage that are part of current law in any Affordable Care Act (also known as Obamacare) replacement bill that is considered by the Senate.
We encourage the Senate to:
- Ensure that people with pre-existing conditions like Down syndrome continue to have access to affordable, high-quality health insurance – regardless of whether or not they currently have insurance;
- Protect federal funding for Medicaid to ensure that people who received coverage under previous expansions won’t lose their insurance;
- Remove caps on federal contributions to state Medicaid programs – caps could result in persons losing coverage or those maintaining Medicaid coverage seeing a reduction in covered medical services and higher out-of-pocket costs; and
- Continue the Affordable Care Act provision that allows children up to age 26 to stay on their parents’ health insurance policies.
Time is of the essence – the Senate may hold a vote on this legislation this week. We urge all Global Down Syndrome Foundation advocates to contact your Senators immediately and urge the Senate to allow for a full and open debate on their healthcare proposal and to oppose any plan that removes current patient protections and coverage for individuals with Down syndrome. As the debate on health care reform continues, Global is engaged with our friends in Congress to protect the health and wellbeing of all individuals with Down syndrome.
Thank you for your advocacy and support!
Corresponding Phone Script:
“Hi. My name is _________ and I live in [Hometown, State].
“I’m a volunteer and advocate with the Global Down Syndrome Foundation. I am deeply concerned that the Senate version of the American Health Care Act will not include protections that are important for people with Down syndrome. In particular, I am concerned that this bill [1) doesn’t guarantee insurance coverage for people with preexisting conditions, 2) cuts federal funding for Medicaid expansion, 3) establishes caps on federal funding for Medicaid, and/or 4) would not allow people to stay on their parents’ health insurance plans up to age 26 – include one or more based on your specific concerns].
“I am also concerned that the public will not have enough time to review and provide feedback on this bill. I hope Senator ____ will work with [his/her] colleagues to make sure that there is ample time for debate and input on this bill.
“These healthcare protections are extremely important not only for people with Down syndrome, but for all Americans.
“Thank you.”
Decoding Dysphagia: Understanding Swallowing Challenges
June 22nd, 2017 by Global Down Syndrome Foundation
From Down Syndrome World Issue 3 of 4

Research shows that more than 50 percent of children with down syndrome who are referred for a swallow study are identified with swallowing problems, also known as dysphagia.
Since dysphagia can impact growth, nutrition, lung health, and participation in regular mealtime experiences, it is important for parents of children with down syndrome to know the potential signs of dysphagia and where to get help if a problem is suspected.
WHAT IS DYSPHAGIA?
Dysphagia can include difficulties in any of the three phases of swallowing:
- The oral phase, when the food/liquid is chewed and/or manipulated in the mouth to make it ready to swallow. Oral phase difficulties can include problems with extracting liquid from a breast, bottle, or cup, chewing, or controlling food/liquid in the mouth.
- The pharyngeal phase, when the food/liquid passes through the throat. Pharyngeal phase difficulties may include delay in starting the swallowing reflex, poor timing of closing off the airway before or during the swallow, and having residual material left in the throat after the swallow. These problems can lead to aspiration or entry of food/liquid into the airway.
- The esophageal phase, when the food/liquid passes from the throat through the esophagus to the stomach. Esophageal difficulties may include food/liquid moving slowly through the esophagus or getting stuck.
 This article was published in the award-winning Down Syndrome World™ magazine. Become a member to read all the articles and get future issues delivered to your door!
This article was published in the award-winning Down Syndrome World™ magazine. Become a member to read all the articles and get future issues delivered to your door!
Signs of dysphagia may include coughing, choking, having red/watering eyes, or sounding congested during or after feeding. Swallowing problems can also be silent, with no obvious signs or symptoms. In children who have frequent upper respiratory illnesses, pneumonia, or persistent oxygen requirement, doctors may suggest having swallowing evaluated, even if there are no clear signs of a problem.
HOW IS DYSPHAGIA DIAGNOSED?
If the child appears to be having problems only in the oral phase of the swallow, a feeding evaluation, during which a child’s feeding skills are observed by a specialist or team of specialists, may be recommended.
If compromised airway protection is suspected, the child’s doctor may order an imaging study. The two most common imaging studies used to diagnose swallowing problems are the videofluoroscopic swallow study (VFSS) and the fiberoptic endoscopic evaluation of swallowing (FEES). The VFSS is done in the radiology department and looks like a “moving X-ray” of the head and neck.
The FEES is typically conducted in the office of an ear, nose, and throat doctor, also known as an otolaryngologist. During the FEES, a small, flexible tube called an endoscope is inserted into the child’s nasal passages. The endoscope is attached to a bright light and a camera, which allow the team to view the inside of the nose and throat.
During the VFSS and the FEES, the swallow team, including a speech-language and/or occupational therapist and a physician (either a radiologist for VFSS or an otolar yngologist for FEES) observes aspects of the child’s swallowing function, such as his or her ability to clear the throat between swallows and protect the airway during swallowing. If a problem is detected, the swallow team may try different strategies to improve swallowing, such as offering a slower-flowing bottle nipple or changing the child’s position.
If difficulties of the esophageal phase of swallowing are suspected, an imaging study completed in radiology called an upper GI or esophagram may be ordered.
HOW CAN I HELP MY CHILD WITH A SWALLOWING PROBLEM?
The most important way that parents and medical providers can help children with dysphagia is to take steps to protect their children’s lungs, as ongoing aspiration can negatively impact pulmonary health. An evaluation with a pulmonologist for further assessment of lung health may be beneficial. Children with severe or persistent dysphagia may be referred to other medical specialists, such as an otolaryngologist or neurologist, for further evaluation as to the cause of the swallowing problem.
Maintaining adequate nutrition and hydration is another critical component of caring for children with swallowing problems. A dietician and/or gastroenterologist may be involved in the child’s care. After the swallow study, the evaluating team will provide recommendations about types of food and liquid that the child is able to swallow most safely. Modifying the child’s diet by minimizing exposure to foods that are more likely to be aspirated and offering foods that can be swallowed safely is an important step that can be taken to give the child the consistent experience of swallowing food and liquid with minimal aspiration.
For children who have severe dysphagia and are unable to swallow any food or liquid without aspirating, providing ongoing positive stimulation to the mouth through play, textured toys, and controlled experiences with small amounts of food and liquid (if approved by the medical team) can help the child maintain and develop skills for using his or her mouth.
Feeding and other developmental therapists can provide helpful services to children with swallowing disorders by teaching skills that support safe and functional feeding and swallowing. Those skills may include teaching the family appropriate positioning and pacing of the mealtime, working on underlying control and strength at the core of the body, and helping children control food or liquid more effectively in the mouth. It is important that therapy for feeding and swallowing issues is individualized for each child and addresses the areas of difficulty identified during the child’s feeding or swallowing evaluation.
PARENT TIPS FOR SWALLOW STUDIES
BEFORE THE STUDY:
- Find out what to expect during the swallow study. For example, will it be a videofluoroscopic swallow study or a fiberoptic endoscopic evaluation of swallowing? Will you be able to feed your child? What will
your child be eating and drinking? - Contact the swallow team ahead of time to make a plan that will work best for your child if you are concerned about whether your child will participate. Many hospitals have child life specialists who can help children be more comfortable during medical tests.
- Be aware that the swallowing team may make recommendations to change your child’s diet to help them swallow more safely.
DURING THE STUDY:
- Help the swallow team to support your child. Bring preferred cups, plates, utensils, foods, and drinks from home. Tell the team if your child has special routines that help him or her eat or drink.
- Make sure you understand the results and recommendations before you leave the appointment. Ask for clarification if you are unsure how to follow the recommendations at home.
AFTER THE STUDY:
- Discuss the results with your child’s doctor and/or medical team.
- Find out who to contact if your swallowing recommendations are not working or if you have follow-up questions.
—-
If your child’s pediatrician recommends a swallow study, visit a medical care center that specializes in treating patients with Down syndrome. Find one at bit.ly/global-medical-care.
About the Authors
Arwen Jackson, M.A., CCC-SLP, and Jennifer Maybee, OTR, M.A., CCC-SLP, are both speech-language pathologists and feeding and sw allowing specialists at the Anna and John J. Sie Center for Down Syndrome at Children’s Hospital Colorado. They work with parents and individuals with Down syndrome to manage dysphagia through the Sie Center’s weekly Feeding Clinic.
References
- Frazier, J. B., and Friedman, B. (1996). Swallow function in children with Down syndrome: a retrospective study. Developmental Medicine & Child Neurology, 38, 695–703.
- Jackson, A., Maybee, J., Moran, M. K., Wolter-Warmerdam, K., and Hickey, F. (2016). Clinical characteristics of dysphagia in children with Down syndrome. Dysphagia, 1–9.
- O’Neill, A. C., and Richter, G. T. (2013). Pharyngeal dysphagia in children with Down syndrome. Otolaryngology – Head and Neck Surgery, 149(1), 146–150.
Like this article? Join Global Down Syndrome Foundation’s Membership program today to receive 4 issues of the quarterly award-winning publication, plus access to 4 seasonal educational Webinar Series, and eligibility to apply for Global’s Employment and Educational Grants.
Register today at downsyndromeworld.org!

















 Experience our inspirational and groundbreaking videos and photos. Our children and self-advocates are beautiful AND brilliant!
Experience our inspirational and groundbreaking videos and photos. Our children and self-advocates are beautiful AND brilliant! Make sure your local Representatives are on the Congressional Down Syndrome Task Force.
Make sure your local Representatives are on the Congressional Down Syndrome Task Force.